Understanding Kidney Function and Its Importance

Intro
The kidneys are often underestimated organs, working silently but diligently behind the scenes to maintain our health. While many focus on heart or brain function, the kidneys play a critical role in ensuring our bodily systems run smoothly. It’s a common misconception that the kidneys only filter blood when, in reality, they are involved in a complex set of functions crucial for homeostasis.
Their primary role is to filter waste from the blood, regulate fluid balance, and balance electrolytes. But there’s more. They also produce hormones that control blood pressure and stimulate the production of red blood cells. Understanding kidney function not only highlights its importance in human health but also underscores the repercussions of any dysfunction. By looking closely at how the kidneys operate, we can appreciate their vital contribution to our overall well-being.
Preamble to Kidney Function
The kidneys are two small, bean-shaped organs located just beneath the ribcage on either side of the spine. They play a monumental role in maintaining overall health by regulating numerous functions, including the body's fluid and electrolyte balance, blood pressure, and waste removal. Understanding how these organs function lays the groundwork for recognizing the significance of renal health in our lives.
In this article, we will explore various aspects of kidney function, focusing on how they contribute to homeostasis, the mechanisms of filtration, and the implications of impaired kidney function. Knowing the essentials about kidney anatomy can significantly enlighten one's approach to health, instilling in us the importance of preserving these vital organs.
Understanding Renal Anatomy
The structure of the kidneys is quite fascinating. Each kidney contains approximately one million nephrons, the microscopic structures responsible for filtering blood. Each nephron itself consists of two main parts: the glomerulus, a tiny network of capillaries, and the renal tubule, which extends to collect and process the filtrate.
Here's a quick look at some key components:
- Cortex: This outer layer contains the glomeruli and parts of renal tubules.
- Medulla: The inner region divided into pyramids, where urine is collected before moving to the pelvis.
- Renal Pelvis: A funnel-shaped structure that channels urine to the ureters.
Understanding these components is crucial, as they illustrate how the kidneys operate in filtration and waste management. A well-functioning renal system ensures that harmful substances are flushed away, and essential nutrients are retained. It's like an intricate dance, where every step is vital.
The Role of Kidneys in Homeostasis
Homeostasis is the body's ability to maintain a stable internal environment despite changes in external conditions. Kidneys contribute to this balance in several ways:
- Fluid Regulation: They adjust the volume of water in the body, preventing dehydration or overload.
- Electrolyte Control: Sodium, potassium, and other electrolytes are carefully regulated to maintain cellular health.
- pH Balance: They help to correct acidosis and alkalosis by excreting hydrogen ions or bicarbonate as needed.
"A small adjustment in kidney function can have rippling effects throughout the entire body, highlighting how interconnected our systems truly are."
"A small adjustment in kidney function can have rippling effects throughout the entire body, highlighting how interconnected our systems truly are."
In essence, kidneys are not mere filters; they're regulators that ensure the body's environment remains conducive to health and function. Without them, the implications could be dire. This foundational knowledge leads us seamlessly into our next section, where we delve deeper into the mechanics of how all of this is accomplished.
Mechanisms of Filtration
The kidneys play a critical role in filtering blood to maintain homeostasis, a balance that is vital for our overall health. Understanding the mechanisms of filtration not only sheds light on how the body regulates essential minerals and waste products but also illustrates the importance of renal health in preventing myriad health issues. Filtration serves as the initial stage in the kidney's sophisticated process for purifying blood, handling the disposal of metabolic waste while retaining what the body needs.
The Glomerular Filtration Process
At the heart of kidney function lies the glomerulus, a tuft of capillaries where the filtration takes place. Blood enters through the afferent arteriole, a large blood vessel bringing oxygen and nutrients. As blood passes through these capillaries, pressure helps to propel small molecules, solutes, and water into the Bowman’s capsule. This initial filtration process is selective, allowing blood cells and large proteins to remain behind while letting smaller particles filter through.
Some key elements at play include:
- Hydrostatic Pressure: This pressure is the driving force that pushes fluid out of the capillaries and into the renal tubule. The higher the pressure, the greater the volume of fluid that is filtered out.
- Selective Permeability: The glomerular membrane selectively allows the passage of materials based on size and charge, ensuring that beneficial components such as proteins are retained in the bloodstream.
- Filtration Rate: The glomerular filtration rate (GFR) is a vital indicator of kidney health. It measures how well the kidneys are filtering blood, which can help to identify potential kidney impairment or disease.
Understanding how this filtration process works is crucial, as disruptions can lead to significant health consequences.
Tubular Reabsorption and Secretion
Once the filtrate enters the renal tubules, a new phase begins: tubular reabsorption and secretion. This part of the renal function is where the kidneys perform their fine-tuning.
- Reabsorption: Essential substances like glucose, amino acids, and electrolytes are selectively reabsorbed into the bloodstream from the renal tubules. This process ensures that valuable nutrients are not lost in the urine.
- Secretion: On the flip side, unwanted substances such as drugs, toxins, and excess ions are secreted into the tubular fluid for excretion.
Both processes work together seamlessly to ensure that the body's biochemical equilibrium is maintained. For instance, if sodium levels dip, the body conserves sodium during reabsorption. Conversely, when saturation occurs, it’s expelled through secretion, thus balancing overall sodium levels.
Role of Nephrons
Nephrons, the functional units of the kidney, are where the magic happens. Each kidney houses around a million nephrons, and each one is involved in filtration, reabsorption, and secretion. They are like tiny recyclers operating in terms of renal function.


- Filtration Unit: Each nephron has a glomerulus for filtration and long tubules for reabsorption and secretion. It's this intricate structure that makes efficient function possible.
- Adjustability: Nephrons can adjust their operation based on the body’s needs, a feature crucial for adapting to fluid intake and hydration levels. This adjustability is influenced by hormones like aldosterone and antidiuretic hormone, allowing the kidneys to react dynamically.
- Compact Structure: The compact arrangement of nephrons within the kidneys allows for efficient filtering and is key in managing metabolic wastes while preserving homeostatic balance.
In summary, the mechanisms of filtration in the kidneys are a complex interplay of processes that ensure the body remains in a state of balance. By understanding these essential aspects, we can appreciate the kidneys' critical role in maintaining health and how any dysfunction can ripple through the body, affecting many other systems.
Regulatory Functions of the Kidneys
The kidneys serve as the body's silent workhorses, tirelessly maintaining internal stability. Their regulatory functions are paramount to our overall health, making it essential to understand the complexities behind them. The kidneys regulate various physiological processes, primarily focused on balancing fluids, electrolytes, and the body's acid-base levels. Each of these roles not only ensures homeostasis but also prevents a range of potential disorders that can arise from any imbalance. Without the kidneys’ diligent efforts, the body would face considerable stress, leading to health issues that could cascade, affecting multiple organ systems.
Fluid and Electrolyte Balance
Balancing fluid and electrolytes is a critical task performed by the kidneys. They do this by filtering blood to remove excess salt and water while retaining what the body needs. This fluid regulation is vital since every single cell in the body depends on having a consistent fluid environment to function properly. If fluid levels, particularly sodium and potassium, swing too far off base, the implications can be dire, leading to conditions like edema or dehydration.
- Here are some key points about fluid and electrolyte balance:
- Sodium Regulation: The kidneys fine-tune sodium levels, which plays a big role in blood pressure regulation. A surge in sodium can lead to increased blood volume, while a decrease can lower blood pressure.
- Potassium Management: Maintaining appropriate potassium levels is crucial for heart function. The kidneys make adjustments in potassium excretion based on dietary intake and hormonal signals.
- Water Homeostasis: The kidneys also concentrate urine, ensuring minimal water loss when the body needs to conserve fluids, such as during exercise or heat exposure.
It’s clear that the kidneys are essential to maintaining fluid balance, as even slight deviations can lead to significant health consequences.
Acid-Base Homeostasis
Another vital function of the kidneys is to regulate the body's acid-base balance. The body's pH level, which must remain close to neutral, can be influenced by various factors like diet, metabolism, and disease. The kidneys help keep the blood pH at around 7.4, a task that involves excreting hydrogen ions and reabsorbing bicarbonate from urine. This delicate process is critical in preventing conditions like acidosis or alkalosis, which can affect nerve function and muscle contractions.
- Several aspects of acid-base homeostasis include:
- Bicarbonate Reabsorption: The kidneys filter out bicarbonate and conserve it to neutralize excess acids in the blood.
- Hydrogen Ion Excretion: By excreting hydrogen ions, kidneys can combat any acidemia, helping to keep the blood from becoming too acidic.
- Ammonia Production: The kidneys produce ammonia as part of their role in excreting acidosis, acting as a buffer to manage hydrogen ions in the urine.
Acid-base homeostasis is not just a minor detail; it’s a keystone of metabolic health. If this balance tilts, it impacts every function in the body, from energy production to cellular repair.
Acid-base homeostasis is not just a minor detail; it’s a keystone of metabolic health. If this balance tilts, it impacts every function in the body, from energy production to cellular repair.
In summary, the kidneys' regulatory roles are far-reaching and intricate. Their fluid-electrolyte balancing acts and their involvement in acid-base homeostasis are vital for maintaining overall body function and health. Understanding these processes offers insights into how we can better care for our kidneys and, consequently, our overall well-being.
Factors Affecting Kidney Function
Understanding the factors that influence kidney function is paramount in grasping how these organs operate and maintain overall health. The kidneys are crucial for filtering waste and managing fluid levels; thus, any disruption can lead to significant health implications. Exploring hydration, diet, and exercise highlights their vital roles in optimizing renal performance.
Impact of Hydration
Water is life, as the saying goes, and it rings particularly true for kidney health. Hydration plays a key role in how well the kidneys can filter blood and eliminate waste products. When a person is well-hydrated, the kidneys can function more efficiently.
Insufficient water intake can lead to concentrated urine, which can stress the kidneys and potentially lead to conditions such as kidney stones. It’s generally recommended that adults consume around 2 to 3 liters of fluid each day, but this can vary based on activity level and climate. Keeping hydration in check is particularly crucial for individuals with existing kidney issues or those prone to urinary tract infections.
"Staying adequately hydrated keeps the body running like a well-oiled machine."
"Staying adequately hydrated keeps the body running like a well-oiled machine."
- Recognizing signs of dehydration, such as darker urine and fatigue, can help ensure proper hydration levels.
- Drinking water regularly, rather than waiting until one feels thirsty, is a good habit.
- Incorporating fruits and vegetables with high water content, like cucumbers and watermelon, can contribute to overall fluid intake.
Diet and Nutritional Influences
A person’s diet can significantly impact kidney health. Nutritional choices can either support or hinder kidney function. Foods high in sodium, for instance, can elevate blood pressure, putting added strain on the kidneys. On the flip side, fruits and vegetables rich in potassium may help balance sodium levels.
- It's key to limit processed foods, which often contain high levels of sodium and unhealthy fats.
- Lean proteins, such as fish and poultry, should replace red meats, which can be harder on kidneys.
- Healthy fats, like those found in avocados and nuts, are beneficial, while sugary drinks should be avoided to prevent sugar spikes that can stress the renal system.
Aside from the nutrient types, meal timing and frequency also matter. Spreading nutrient intake across several smaller meals can help manage blood sugar levels, further decreasing the kidneys' workload.
Exercise and Its Effects
Physical activity is another critical element influencing kidney function. Regular exercise can help maintain a healthy weight, lower blood pressure, and improve overall well-being. Obesity is linked to increased risk of kidney disease, highlighting the importance of maintaining an active lifestyle.
- Engaging in moderate exercise, such as brisk walking or swimming, is beneficial.
- Activities should be tailored to individual capacity; what matters is consistency rather than intensity.
- Strength training can also help improve muscle mass and boost metabolism, which in turn can positively affect kidney health by regulating blood sugar and pressure levels.


Ultimately, a balanced approach that encompasses hydration, nutrition, and exercise can provide the best support for kidney function, allowing the kidneys to do their job effectively and keeping the rest of the body in a state of balance.
The Consequences of Impaired Kidney Function
Understanding the consequences of compromised kidney function is pivotal not just for those interested in nephrology, but for anyone keen on maintaining their health. The kidneys, though small in size relative to body weight, have immense responsibilities. They filter waste, balance fluids, and regulate electrolytes, making their efficient operation crucial for homeostasis. When their function diminishes, the repercussions can be severe, affecting overall health significantly. This section lays bare the various forms of kidney impairment, illustrating their implications in everyday life and healthcare.
Acute Kidney Injury
Acute Kidney Injury (AKI) is a sudden, often reversible, decline in kidney function that can stem from numerous causes, such as dehydration, infections, or certain medications. Recognizing AKI is essential, as timely diagnosis can forestall lasting damage.
Key Aspects of AKI:
- Rapid Onset: Symptoms can appear abruptly, frequently within hours or days.
- Causes: Common triggers include sepsis, significant blood loss, and nephrotoxic drugs.
- Diagnosis: Blood tests revealing elevated creatinine levels aid in identifying AKI.
The ramifications of AKI can manifest not just in the kidneys but also affect other organs due to toxin accumulation in the bloodstream. This is why patients presenting with symptoms—like decreased urine output or swelling in legs—need immediate medical evaluation.
Chronic Kidney Disease
Chronic Kidney Disease (CKD) unfolds gradually and can progress to the advanced stages where kidney function is severely impaired. Its long-term nature means many people may not even realize they have it until significant damage is done.
Characteristics of CKD:
- Staging: CKD is divided into five stages based on the Glomerular Filtration Rate (GFR), with Stage 1 being mild dysfunction and Stage 5, or end-stage renal disease, requiring dialysis or transplantation.
- Symptoms: Patients may experience fatigue, fluid retention, and frequent urination, especially at night.
- Risk Factors: These include diabetes, hypertension, and family history.
The insidious nature of CKD means that regular check-ups can be beneficial for early detection. Proper management, including lifestyle adaptations and medication, can often slow the progression significantly.
End-Stage Renal Disease
End-Stage Renal Disease (ESRD) represents the terminal phase of CKD, where the kidneys function at less than 15% of their capacity. At this juncture, patients require renal replacement therapies—either dialysis or a kidney transplant—to survive.
Understanding ESRD:
- Dialysis: This procedure artificially removes waste products and excess fluid from the blood. There are two main types—hemodialysis and peritoneal dialysis.
- Transplantation: A healthy kidney from a donor is surgically placed to restore function.
- Life-Altering Choices: Managing ESRD often requires extensive lifestyle changes, like dietary modifications and adhering to a strict medication regimen.
The transition to ESRD often feels overwhelming. The chronic physical demands, emotional burden, and financial implications can be daunting.
"Early detection and proactive management of kidney issues can significantly change the quality of life for those at risk."
"Early detection and proactive management of kidney issues can significantly change the quality of life for those at risk."
In sum, understanding the stages and implications associated with Acute Kidney Injury, Chronic Kidney Disease, and End-Stage Renal Disease highlights the importance of kidney health in broader human well-being. It is not merely about preventing ailments but enhancing quality of life through preventive measures, timely diagnosis, and effective treatments.
Diagnostic Approaches to Assess Kidney Function
Assessing kidney function is critical in various medical contexts. Given the pivotal role of the kidneys in maintaining homeostasis, understanding their functionality helps to detect potential issues before they turn into serious conditions. Various diagnostic measures are utilized to evaluate kidney health, each having distinct elements and benefits. These methods help create a comprehensive picture of kidney function, aiding in diagnosis, treatment, and management of renal health.
Blood Tests and Markers
Blood tests offer a straightforward means to evaluate kidney function. Two primary markers are routinely assessed: creatinine and blood urea nitrogen (BUN).
- Creatinine is a waste product generated from muscle metabolism. Normal kidneys filter out this substance effectively; elevated levels may indicate impaired renal function.
- BUN, on the other hand, measures the amount of nitrogen in the blood that comes from urea, another byproduct of protein metabolism. High BUN levels might suggest that the kidneys are not working properly, though diet, hydration, and other factors can also influence these results.
It's not just about numbers. Understanding the ratios of these markers can provide insights into whether the problem lies within the kidneys or perhaps in other organs. For example, a high BUN to creatinine ratio could suggest pre-renal azotemia, which occurs before the kidneys in the circulatory system, indicating issues like dehydration or heart failure. Regular monitoring through blood tests can empower healthcare providers to make informed decisions about treatment approaches.
Urine Analysis Techniques
Urine analysis acts as another vital tool for diagnosing kidney issues, particularly through urinalysis. This involves examining the physical, chemical, and microscopic aspects of urine to identify abnormalities.
- Physical Examination: This looks for color, clarity, and specific gravity, giving immediate clues about hydration and concentration.
- Chemical Testing: Testing for various substances can reveal infections, drug influences, and signs of kidney disease. For instance, protein in urine (proteinuria) can be a significant indicator of kidney damage.
- Microscopic Examination: This involves looking for cells, crystals, and bacteria under a microscope. The presence of red blood cells can point to glomerulonephritis or damage to kidney tissues.
Urine tests are generally non-invasive and can sometimes provide quicker results, making them valuable in both outpatient settings and when quick assessments are needed.
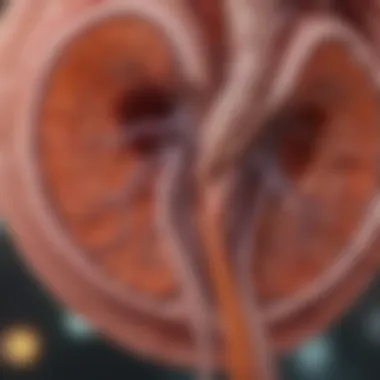

Imaging Studies
Imaging studies supplement blood and urine tests, offering a more visual approach to assessing kidney health. Types of imaging include ultrasound, CT scans, and MRIs.
- Ultrasound: This is often the first step in renal imaging. It allows for real-time assessment of kidney structure and blood flow without exposing the patient to radiation. The kidneys appear as dark crescents filled with fluid, highlighting any obstructions or size discrepancies.
- CT Scans: With cross-sectional imaging, these scans afford a more detailed view of the kidneys and surrounding tissues. They help identify cysts, tumors, or structural abnormalities that might not be easily viewed by ultrasound.
- MRIs: Although less commonly used for kidneys than other organs, MRIs are valuable for assessing complex structures or diseases affecting blood vessels and soft tissues around the kidneys.
In essence, these imaging techniques serve to fortify the findings from blood and urine tests, crafting a multifaceted understanding of kidney function.
"Effective kidney assessments combine various methods, offering a robust diagnostic approach that is crucial in patient care."
"Effective kidney assessments combine various methods, offering a robust diagnostic approach that is crucial in patient care."
Advancements in Treatments and Interventions
The innovations in kidney treatments and interventions hold immense significance for patients grappling with renal issues. These advancements not only enhance survival rates but also improve the quality of life for those managing chronic kidney diseases or experiencing acute complications. By illuminating the path toward earlier detection and tailored therapies, this section emphasizes the critical nature of such advancements in the broader context of human health. As life expectancy increases, the prevalence of diabetes and hypertension has grown, both of which are notorious culprits in kidney dysfunction. Thus, the need for effective treatments and proactive health management is paramount.
Lifestyle Modifications
Lifestyle choices can either bolster or hinder kidney health. Being mindful of dietary habits is crucial; a diet low in sodium, processed sugars, and unhealthy fats supports kidney function. Incorporating fresh fruits, vegetables, and whole grains can transform one’s renal wellbeing.
Aside from nutrition, hydration plays a vital role in renal health. Drinking sufficient water helps the kidneys remove waste and toxins. However, individual hydration needs can vary based on organ functions and overall health, stressing the importance of personalized hydration strategies.
Regular physical activity also contributes to better kidney health. Engaging in aerobic exercises like brisk walking or cycling can take a load off the kidneys, improving blood circulation and effectively managing blood pressure. Overall, lifestyle modifications can not only delay the progress of kidney diseases but also reduce potential complications.
Pharmacological Interventions
Medications have made significant strides in treating kidney-related ailments. Drugs like angiotensin-converting enzyme (ACE) inhibitors play a pivotal role in managing conditions like hypertension and heart failure, which can indirectly support kidney function. The mechanism involved helps relax blood vessels, hence reducing blood pressure; this in turn lessens the burden on the kidneys.
Furthermore, the use of sodium-glucose cotransporter-2 (SGLT2) inhibitors has transformed the landscape of treatment for diabetic kidney disease. These medications lower blood sugar levels and reduce hyperfiltration in the kidneys. Patients on these drugs have reported slower progression of kidney disease and fewer necessary interventions for managing diabetes.
While pharmacological treatments dramatically improve outcomes, they also necessitate regular monitoring for potential side effects.
Dialysis and Transplantation Options
For individuals approaching end-stage renal disease, dialysis becomes a crucial option. This treatment substitutes the kidney's filtering function, removing waste, excess water, and toxins from the blood. Two primary types of dialysis exist: hemodialysis, where blood is filtered through a machine, and peritoneal dialysis, which uses the lining of the abdomen for filtration. Patients often have to balance between lifestyle and treatment frequency, as these can significantly affect their daily routines.
Transplantation offers another formidable option, providing a more permanent solution for renal failure. The challenge, however, lies in finding compatible donor organs, which is an ongoing struggle for many. Post-surgery, patients must adhere to a rigorous immunosuppressive regimen to prevent organ rejection. However, the long-term benefits can be immense, leading to a significant improvement in life quality and longevity compared to remaining on dialysis.
In summary, advancements in treatments and interventions for kidney health are evolving, driven by both lifestyle modifications and medical innovations. These developments are critical for managing kidney diseases more effectively while improving the outlook for those affected.
"A proactive approach to kidney health combines innovative treatments with sustainable lifestyle choices to ensure a better quality of life and overall wellbeing."
"A proactive approach to kidney health combines innovative treatments with sustainable lifestyle choices to ensure a better quality of life and overall wellbeing."
By keeping abreast of these advancements, patients, healthcare professionals, and researchers can work collectively toward improved outcomes in renal health.
Epilogue
The final thoughts on kidney function weave together the intricate tapestry of health, emphasizing the vital role these organs play not only in filtering waste but also in maintaining homeostasis. Understanding how kidneys operate helps illuminate their importance not merely as waste-processing machines but as essential players in our overall health management. This wraps the concepts presented, linking together how renal physiology impacts various body systems.
Reflections on Kidney Health
When we reflect on kidney health, it is evident how often we take these organs for granted. Most people don’t give their kidneys a second thought until an issue arises. Just as we pay attention to our heart and lungs, it’s crucial to be just as mindful of our kidneys. They have a hand in so many processes: regulating blood pressure, balancing electrolytes, and producing essential hormones.
"Our kidneys don’t just filter; they play a pivotal role in our metabolic harmony."
"Our kidneys don’t just filter; they play a pivotal role in our metabolic harmony."
Many factors influence renal health, from diet to hydration and even stress levels. A typical Western diet, often high in processed foods and sodium, can wreak havoc on kidney function over time. It invites conditions such as hypertension and diabetes, leading to chronic kidney issues. Likewise, inadequate fluid intake can turn the kidneys into a straw trying to suck up nutrients without sufficient support. By fostering an awareness of what we consume and how we live, we enhance our kidney health.
Encouraging Healthy Practices
Encouraging healthy practices is essential in staving off disorders that may afflict the urination system. Here are some simple yet effective strategies:
- Stay Hydrated: Drinking enough water supports optimal filtration and helps prevent kidney stones. Aim for around 2 liters daily, adjusting for activity levels and climate.
- Balanced Diet: Incorporate fresh fruits, vegetables, and whole grains. Limit salt and saturated fat intake, as they can put extra pressure on the kidneys.
- Regular Exercise: Engaging in physical activity can help maintain a healthy weight, directly influencing kidney function. Exercise improves blood circulation and reduces the risk of hypertension.
- Routine Check-ups: Regular health screenings help catch issues early, especially if you have pre-existing conditions.
By adopting these practices, we create a nurturing environment for our kidneys. Awareness that simple lifestyle choices can dramatically impact renal health should echo in our daily routines. Normalizing kidney health discussions will not only enhance our focus but also encourage proactive measures to safeguard these vital organs.







